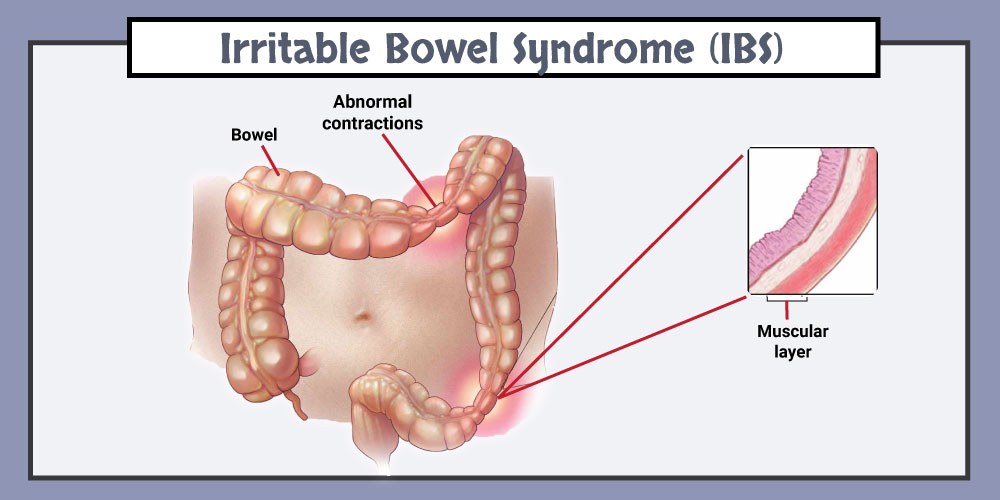
Irritable bowel syndrome(IBS) or irritable bowel disease(IBD) is a long-term gastrointestinal disorder. It causes abdominal pain, bloating, mucous in stools, irregular bowel habits, and alternating diarrhea and constipation.
IBS can cause persistent discomfort, but most people will not experience severe complications.
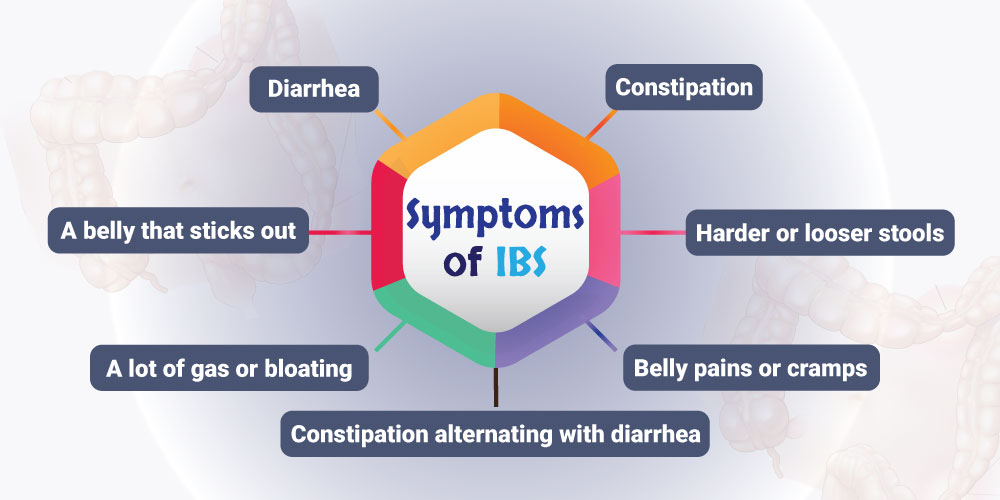
What Are Symptoms of IBS?
The most common symptoms experienced by people with IBS are:
- Diarrhea
- Constipation
- Constipation alternating with diarrhea
- Belly pains or cramps, usually in the lower half of the belly, that get worse after meals and feel better after a bowel movement
- A lot of gas or bloating
- Harder or looser stools
- A belly that sticks out
Symptoms often worsen after eating. A flare-up may last from 2 to 4 days, and then symptoms may either improve or go away completely.
What Is The Right Diet for IBS?
Dietary factors can play a role. Symptoms are often worse after consuming certain products, such as chocolate, milk, or alcohol. There may be either constipation or diarrhea.
Some fruits, vegetables, and sodas can trigger bloating and discomfort. It is unclear whether a food allergy or intolerance plays a role.
Common dietary triggers of cramping or bloating include:
- foods that cause flatulence, such as beans, celery, onions, carrots, raisins, bananas, apricots, prunes, brussel sprouts, pretzels, and bagels
- dairy products
- sugar-free gum
- some candies
- products with caffeine in them, maybe due to lactose (sugar), sorbitol, or caffeine intolerance, rather than IBS
Fiber: Some people with IBS need to increase their fiber intake, while others have to consume less. A properly balanced level of fiber in the diet can help promote healthy digestion.
Probiotics: These may help some people. The benefits take about 4 weeks to appear.
Food diary: Keeping a record of foods eaten and their effect will help identify the major trigger foods.
Changes in eating habits can help control symptoms. There is no IBS diet that works for everybody, so the person may need to go through a process of trial and error to achieve an optimum diet.
What Are The Causes of IBS?
It is unclear what causes IBS, but it is not contagious or cancer-related.
Factors that may be involved include:
- diet
- environmental factors, such as stress
- genetic factors
- hormones
- digestive organs being excessively sensitive to pain
- an unusual response to infection
- a malfunction in the muscles used to move food through the body
- an inability of the central nervous system(CNS) to control the digestive system properly
A person’s mental and emotional state may have an impact. People who have had a traumatic experience have a higher risk of developing IBS.
Coping With IBS Effectively
As the causes are uncertain, treatment for IBS aims to relieve symptoms and improve quality of life.
This usually involves some dietary and lifestyle changes, as well as learning how to manage stress.
The following may help:
- avoiding sorbitol, found in some chewing gums, diet foods, and sugar-free sweets, as it can cause diarrhea
- consuming more oat-based foods to reduce gas or bloating
- not skipping meals and eating at the same time every day
- eating slowly
- limiting alcohol intake
- avoiding carbonated sugary beverages, such as soda
- limiting the intake of certain fruits and vegetables
- limiting tea and coffee intake to three cups per day
- drinking enough fluids, at least eight cups of fluid per day for most people
It may help to avoid or limit the intake of resistant starch, commonly found in processed or recooked foods and in some legumes. Resistant starch is not broken down in the digestive tract and counts as a component of dietary fiber.
Risk factors of IBS
The following groups of people are more likely to have IBS:
- Younger adults: IBS affects people of all ages, but diagnosis usually occurs before the age of 45 years, often at 20 to 30 years.
- Gender: It is more likely to affect women.
- Family history: If a close relative has or has had IBS, there may be a higher chance of developing it. However, there is no clear link.
- Environment: Ongoing research is investigating whether the family-history risk of IBS is linked to genes, a shared family environment, or both.